The Hidden Effects of Saturated Fat on Your Blood Glucose, Cholesterol, Blood Pressure, and Mitochondria
By Cyrus Khambatta, PhD
If you've ever been told that saturated fat is "fine in moderation" or that the saturated fat debate has been "debunked," I understand the confusion. The nutrition world is full of contradictory headlines, and it can feel impossible to know what's actually true.
So let's do what we always do here – go straight to the research and let the data speak for itself.
Because when you look at the totality of the evidence – not just one cherry-picked study, but the full body of randomized controlled trials, systematic reviews, and mechanistic research – a clear picture emerges:
Saturated fat has measurable, well-documented effects on insulin sensitivity, blood glucose regulation, cholesterol metabolism, blood pressure, and mitochondrial function.
And understanding how it does this at the cellular level is the key to making informed decisions about what you put on your plate.
Saturated Fat Impairs Insulin Resistance
Let's start with one of the most important (and most misunderstood) effects of saturated fat: saturated fat significantly reduces insulin sensitivity.
A controlled feeding study published in the European Journal of Nutrition by von Frankenberg et al. put overweight and obese adults on either a high-fat, high-saturated fat diet (55% fat, 25% saturated fat) or a low-fat diet (20% fat, 8% saturated fat) for four weeks. All food was provided, and calorie intake was carefully controlled to keep body weight stable.
The results were striking: the high-fat, high-saturated fat diet significantly decreased insulin sensitivity even though participants didn't gain any intra-abdominal fat.
This is a critical finding because it tells us that saturated fat doesn't need to make you gain belly fat to impair how your cells respond to insulin. The damage happens at the cellular level, independent of weight change.
A landmark review by Riccardi et al. in Clinical Nutrition confirmed this pattern across multiple study designs: saturated fat significantly worsens insulin resistance, while monounsaturated and polyunsaturated fatty acids improve it – in part through modifications in cell membrane composition that reflect dietary fat intake.
And a comprehensive systematic review and meta-analysis of 102 randomized controlled feeding trials by Imamura et al., published in PLOS Medicine, found that replacing saturated fat with polyunsaturated fat (PUFA) significantly lowered blood glucose, HbA1c, C-peptide, and HOMA-IR – a key marker of insulin resistance. PUFA also improved insulin secretion capacity, whether it replaced carbohydrate, saturated fat, or even monounsaturated fat.
The takeaway? The type of fat you eat directly influences how well muscle and liver cells respond to insulin.
The Biological Mechanisms of Ceramides, Diacylglycerol, and Lipotoxicity
So what's actually happening inside muscle cells when you eat a diet high in saturated fat?
The mechanism here is well-characterized. When saturated fatty acids (particularly palmitate, the most common saturated fat in the Western diet) enter muscle cells in excess, they don't just get stored as “neutral” fat.
Instead, saturated fatty acids get converted into toxic lipid intermediates, primarily ceramides and diacylglycerol (DAG).
A 2024 review published in Drug Design, Development and Therapy by Elkanawati et al. synthesized findings from both human and animal studies and confirmed that intramyocellular lipid metabolites (especially those derived from saturated fat) play a central role in mediating insulin resistance.
The fat composition within muscle tissue, particularly the proportion of saturated fat, has a direct impact on how well insulin signaling works.
For the super nerds, here's the biochemical cascade:
DAG activates protein kinase C (PKC), which then impairs insulin signaling by phosphorylating insulin receptor substrate-1 (IRS-1) at the wrong sites – essentially putting the brakes on insulin's ability to tell your cells to take up glucose.
Ceramides inhibit Akt/PKB, a critical enzyme in the insulin signaling pathway. When Akt is suppressed, glucose uptake into muscle cells slows down, and blood glucose rises.
Ceramides also cause endoplasmic reticulum stress and mitochondrial dysfunction, both of which further contribute to insulin resistance.
What's particularly interesting is that monounsaturated fats like oleate don't trigger this cascade. Research by Chavez et al. demonstrated that exposing muscle cells in vitro to saturated fatty acids (but not monounsaturated fatty acids) inhibited insulin signaling. And when researchers blocked ceramide synthesis, the insulin-impairing effects of saturated fat were completely negated.
A 2024 review by Sergi et al. in Nutrition Research Reviews went further, showing that total dihydroceramides – precursors to ceramides – were elevated up to 9 years before a diagnosis of type 2 diabetes, suggesting that ceramide accumulation isn't just a consequence of insulin resistance. It may be one of the earliest warning signs.
In short: saturated fat promotes the accumulation of ceramides and DAG in muscle tissue, which directly impairs insulin signaling and sets the stage for chronically elevated blood glucose.
Saturated Fat Impairs Mitochondrial Function
Mitochondria are the engines that convert the food you eat into usable energy (ATP). When they're functioning well, you feel energized, your blood sugar stays stable, and your metabolism hums along efficiently.
But when mitochondria are exposed to an excess of saturated fatty acids, the research shows that they become less efficient and generate more free radicals – reactive molecules that damage DNA, proteins, and lipid membranes.
For the super nerds, here's the mechanism that involves several interconnected pathways:
Saturated fat overloads mitochondrial fatty acid oxidation, leading to incomplete combustion and the generation of acylcarnitines – metabolic byproducts that signal impaired fat burning.
The breakdown products of saturated fats include lipid peroxides and aldehydes, which directly damage mitochondrial membranes and impair the electron transport chain.
Damaged mitochondria generate more free radicals, creating a vicious cycle: oxidative stress leads to more mitochondrial dysfunction, which leads to more oxidative stress.
This is the cellular equivalent of running a car engine on contaminated fuel. The engine doesn't just slow down – it starts producing exhaust that corrodes its own parts.
Elkanawati et al. confirmed that high-fat diets – particularly those rich in saturated fat – disrupt insulin signaling and increase inflammation through these lipid mediators, with ceramides playing a dual role: impairing both insulin signaling and mitochondrial function simultaneously.
The practical implication is clear: a diet chronically high in saturated fat doesn't just affect your blood glucose. It compromises the fundamental energy-producing machinery.
Saturated Fat and Cholesterol: A More Nuanced Picture Than You've Been Told
Now let's talk about cholesterol – because this is where the conversation gets genuinely interesting.
The data clearly shows that saturated fat raises LDL cholesterol. This is well-established and isn't seriously debated in the scientific community. A WHO report by Mensink confirmed that replacing saturated fat with monounsaturated fat, polyunsaturated fat, or carbohydrates reduces both total cholesterol and LDL cholesterol.
But here's where it gets nuanced: does lowering LDL cholesterol through saturated fat reduction actually prevent heart attacks and cardiovascular death?
A systematic review and meta-analysis of randomized controlled trials by Yamada et al., published in the JMA Journal in 2025, analyzed nine RCTs involving 13,532 participants and found no significant differences in cardiovascular mortality, all-cause mortality, myocardial infarction, or coronary artery events between groups that reduced saturated fat and those that didn't.
The authors concluded: "The findings indicate that a reduction in saturated fats cannot be recommended at present to prevent cardiovascular diseases and mortality."
Now, before you take that as a green light to eat unlimited butter and bacon, let me add some important context.
First, 7 of the 9 trials in that meta-analysis were secondary prevention studies – meaning participants already had heart disease. And 8 of the nine trials were conducted before statins were widely available. So the question of whether saturated fat reduction adds benefit on top of modern medical care remains unanswered.
Second, a separate systematic review by Hooper et al. found that replacing saturated fat with polyunsaturated fat does lower coronary heart disease events – even if it doesn't significantly reduce cardiovascular mortality. And replacing saturated fat with refined carbohydrates (sugar and starch) actually increases events.
The bottom line on cholesterol: saturated fat raises LDL, and replacing it with polyunsaturated fat appears to reduce cardiovascular events. But simply cutting saturated fat without paying attention to what replaces it won't necessarily protect your heart.
This is why we teach our clients to focus on the quality of their entire dietary pattern – not just the removal of one macronutrient.
Saturated Fat Increases Blood Pressure and Oxidative Stress
The relationship between saturated fat and blood pressure is mediated through several pathways, including its effects on endothelial function, inflammation, and insulin resistance itself.
Riccardi et al. noted that shifting from saturated to monounsaturated fat intake reduces diastolic blood pressure, while omega-3 fatty acids reduce blood pressure in people with hypertension.
The mechanism here is tied to endothelial health. Saturated fat promotes oxidative stress in the vascular endothelium – the thin layer of cells lining your blood vessels. When endothelial cells are exposed to chronic oxidative stress, they produce less nitric oxide (NO), a molecule that relaxes blood vessels and keeps blood pressure in a healthy range.
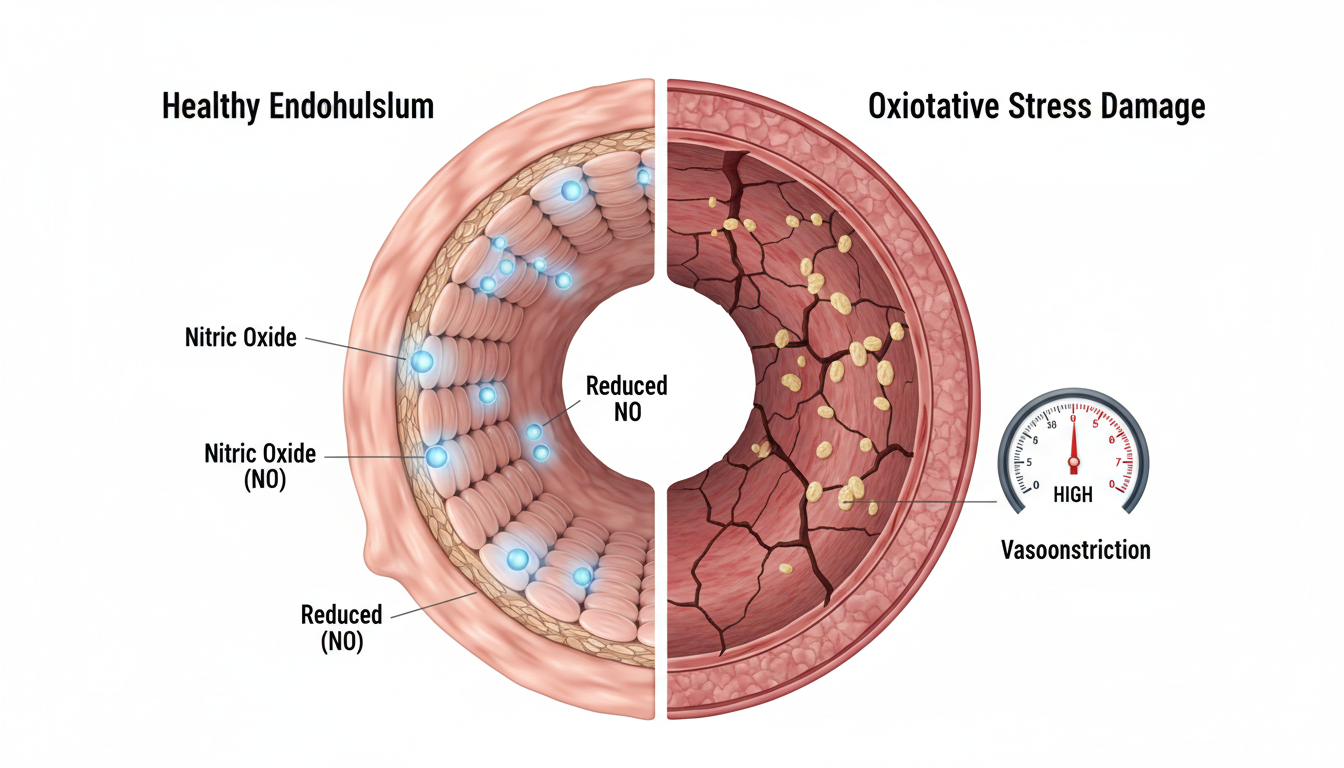
Additionally, the insulin resistance caused by saturated fat has its own blood pressure-raising effects. Insulin resistance leads to:
Increased sodium retention in the kidneys
Elevated sympathetic nervous system activity
Impaired nitric oxide-mediated vasodilation
All of these contribute to elevated blood pressure over time. This is why insulin resistance and hypertension so frequently travel together – they share common upstream drivers, and saturated fat is one of them.
What This Means for You
If you're reading this and feeling overwhelmed, I want you to take a step back and see the bigger picture.
The research isn't telling you that a single pat of butter will give you diabetes. What it is telling you is that a dietary pattern chronically high in saturated fat creates a cascade of metabolic effects – from ceramide accumulation in muscle tissue, to impaired mitochondrial function, to elevated LDL cholesterol, to compromised endothelial function – that collectively increase your risk for insulin resistance, type 2 diabetes, cardiovascular disease, and hypertension.
And here's the optimistic part: these effects are very reversible.
When you replace saturated fat with polyunsaturated fat, monounsaturated fat, and fiber-rich whole foods, the research consistently shows improvements in:
Insulin sensitivity (via reduced ceramide and DAG accumulation)
Blood glucose regulation (via improved mitochondrial function)
LDL cholesterol (via changes in hepatic cholesterol metabolism)
Blood pressure (via improved endothelial function and nitric oxide production)
Your body has a remarkable capacity to heal when you give it the right fuel. The key is understanding that lifestyle should always be the first line of defense when trying to overcome chronic metabolic conditions – not a pharmaceutical band-aid that masks symptoms without addressing root causes.
That doesn't mean medications don't have a time and a place. They absolutely do. But the foundation of metabolic health is, and always will be, what you eat, how you move, how you sleep, and how you manage stress.
What We Recommend
At Evolution Health, we help our clients engineer their dietary fat intake with precision – reducing saturated fat from animal products and refined oils while increasing intake of whole food sources of polyunsaturated and monounsaturated fats like nuts, seeds, avocados, and omega-3-rich foods.
Combined with a fiber-rich, antioxidant-dense, plant-forward eating pattern, this approach addresses the root causes of insulin resistance, high cholesterol, high blood pressure, and mitochondrial dysfunction – all at once.
If you're ready to take control of your metabolic health using evidence-based strategies that actually work, click here to schedule a free strategy session with our team. We'll show you exactly how to build a lifestyle that reverses chronic inflammation from the inside out.
Scientific References
von Frankenberg AD, Marina A, Song X, et al. A high-fat, high-saturated fat diet decreases insulin sensitivity without changing intra-abdominal fat in weight-stable overweight and obese adults. Eur J Nutr. 2017;56(1):431-443. PubMed
Riccardi G, Giacco R, Rivellese AA. Dietary fat, insulin sensitivity and the metabolic syndrome. Clin Nutr. 2004;23(4):447-456. PubMed
Imamura F, Micha R, Wu JHY, et al. Effects of Saturated Fat, Polyunsaturated Fat, Monounsaturated Fat, and Carbohydrate on Glucose-Insulin Homeostasis: A Systematic Review and Meta-analysis of Randomised Controlled Feeding Trials. PLOS Medicine. 2016;13(7):e1002087. PLOS Medicine
Elkanawati RY, Sumiwi SA, Levita J. Impact of Lipids on Insulin Resistance: Insights from Human and Animal Studies. Drug Des Devel Ther. 2024;18:3337-3360. PMC
Chavez JA, Knotts TA, Wang LP, et al. A role for ceramide, but not diacylglycerol, in the antagonism of insulin signal transduction by saturated fatty acids. J Biol Chem. 2003;278(12):10297-10303. PubMed
Sergi D, Zauli E, Celeghini C, et al. Ceramides as the molecular link between impaired lipid metabolism, saturated fatty acid intake and insulin resistance. Nutr Res Rev. 2024;38(1). Cambridge Core
Cuthbertson DJ, Babraj J, Mustard KJ, et al. Key role for ceramides in mediating insulin resistance in human muscle cells. J Biol Chem. 2007;282(17):12583-12589. PubMed
Kennedy A, Martinez K, Chuang CC, et al. Saturated fatty acid-mediated inflammation and insulin resistance in adipose tissue: mechanisms of action and implications. J Nutr. 2009;139(1):1-4. PubMed
Yamada S, Shirai T, Inaba S, et al. Saturated Fat Restriction for Cardiovascular Disease Prevention: A Systematic Review and Meta-analysis of Randomized Controlled Trials. JMA J. 2025;8(2):395-407. JMA Journal
Hooper L, Martin N, Jimoh OF, et al. A systematic review of the effect of dietary saturated and polyunsaturated fat on heart disease. Nutr Metab Cardiovasc Dis. 2017;27(12):1060-1080. PubMed
Lytrivi M, Gomes Da Silveira Cauduro C, Kibanda J, et al. Impact of saturated compared with unsaturated dietary fat on insulin sensitivity, pancreatic β-cell function and glucose tolerance: a systematic review and meta-analysis of randomized, controlled trials. Am J Clin Nutr. 2023;118(4):739-753. ScienceDirect
Summers SA, Garza LA, Zhou H, Birnbaum MJ. Characterizing the effects of saturated fatty acids on insulin signaling and ceramide and diacylglycerol accumulation in 3T3-L1 adipocytes and C2C12 myotubes. Arch Biochem Biophys. 2003;419(2):101-109. PubMed
Lower LDL Cholesterol Naturally with Food: Simple Ways to Add Proven LDL Reducers to Your Everyday Routine (Audible Audio Edition): Michael Greger MD, Kristine Dennis, Michael Greger MD, NutritionFacts.org: Books [Internet]. [cited 2026 Feb 24].

